When people talk about hormones, it’s often in relation to how they affect things like mood and energy levels, PMS symptoms, libido, and metabolism. But the truth is, these vital chemical messengers can have a profound effect on your skin, too. If you’ve ever dealt with hormonal acne you’re probably well aware of this, but your changing hormone levels throughout life have just as big of an effect.
The shift in sex hormones that occur as women age (and even throughout a single menstrual cycle!) can impact everything from sebum production, barrier function, collagen and hyaluronic acid production, and more.
The good news: Understanding how your short-term and long-term hormonal shifts influence your skin can help you target your skincare routine and lifestyle habits to support optimal skin health and appearance. Below, we cover the hormonal shifts you can expect to experience throughout your lifetime and simple, expert-approved strategies to help manage them.
The Key Players: How 3 Different Hormones Affect Skin

Before we dive into how hormones shift throughout a woman’s life—and what that means for skin health—it’s helpful to understand how specific sex hormones impact your skin. As with most other cells in your body, various types of cells within your skin have receptors for different hormones, and the presence or absence of these hormones can lead to different skin manifestations.
While non-sex hormones such as cortisol (a stress hormone) can impact the skin, to an extent, we’ll hone in on the ones that make the biggest difference: estrogen, progesterone, and androgens.
Estrogen
“Estrogen is key for the normal functioning of the skin as well as the blood vessels, hair follicles, oil glands, and our pigment-producing cells called melanocytes,” says Keira Barr, MD, a dual board-certified dermatologist and menopause specialist and author of The Skin Whisperer. “It is associated with collagen production, increased skin thickness, increased hyaluronic acid production, improved skin barrier function, maintaining skin hydration, reduced sebaceous (oil) gland activity, and improved wound healing. It also plays a role in modulating inflammation.”
Progesterone
The effect of progesterone on the skin is less well defined, but, according to Dr. Barr, it’s thought to contribute to skin elasticity, pigmentation, and the increased circulation and sebaceous gland activity that is observed in the second half of the menstrual cycle.
Androgens
Androgens, which are normally thought of as male hormones, can also impact women’s skin. These hormones, including testosterone, are produced in small amounts by the female body and play a role in oil gland production. When hormones are imbalanced—as can occur in women with PCOS and when women experience comparatively elevated androgen levels during menopause—androgens may also contribute to unwanted facial hair growth.
In your 20s and 30s
A lot can be going on in your 20s and 30s. Acne, which is often associated with adolescence, can still affect many women during this time period, and it can have a lot to do with the hormonal shifts that occur during womens’ monthly cycles. In fact, research shows that about 50 percent of women in their 20s and 35 percent of women in their 30s experience acne.
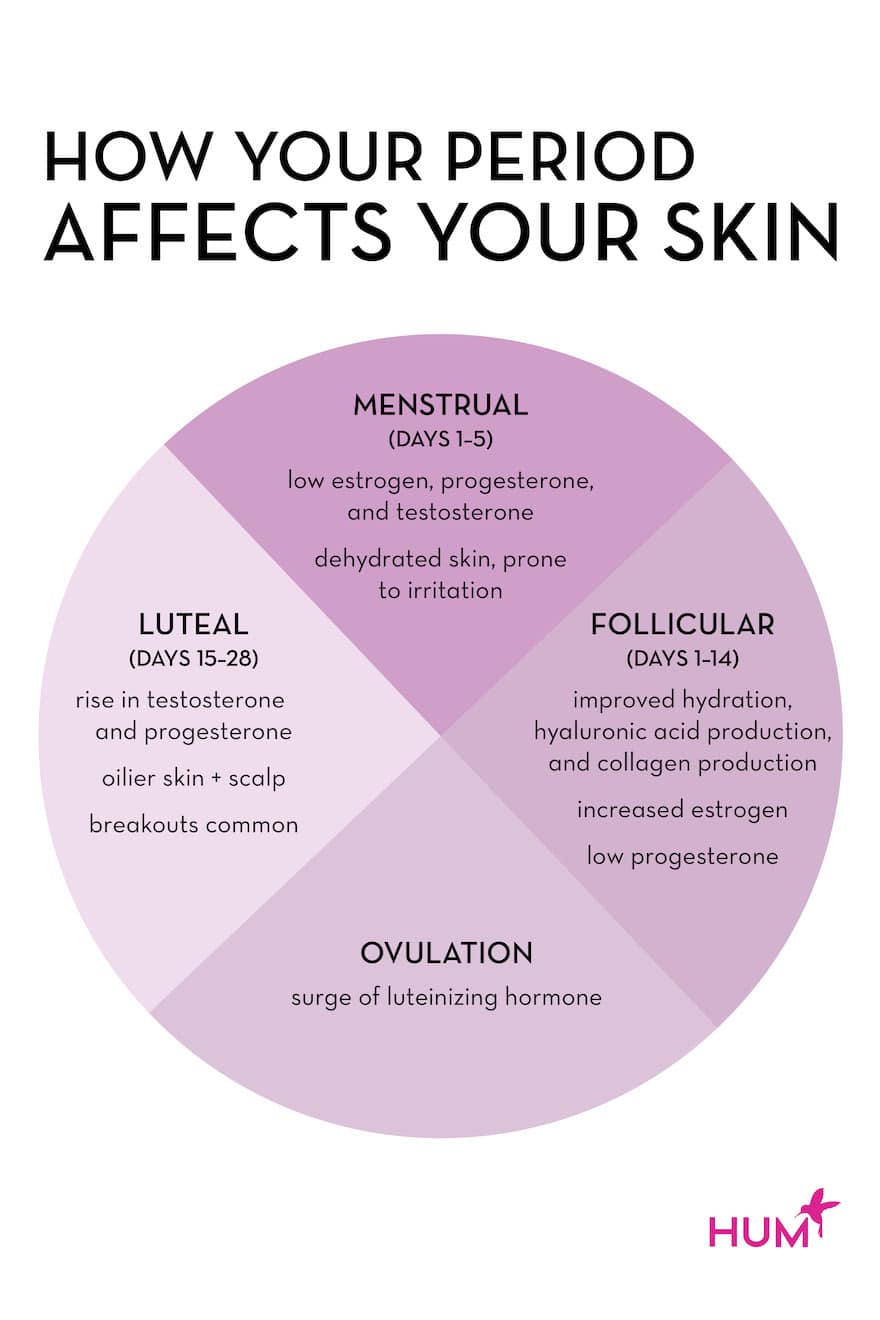
But in addition to periodic bouts of acne, skin can also vary in its moisture content, sensitivity, and general radiance depending on the time of the month. Here, we break down the typical hormonal changes that occur throughout a menstruating woman’s cycle, how they affect skin, and what you can do about it:
Menstruation (days 1-5)
Each menstrual cycle starts with menstruation, or your period. This takes place in the very beginning of the follicular phase. “During this phase, levels of estrogen are at their lowest, which translates to a decrease in skin hydration and vulnerability of the skin barrier to irritation and inflammation,” says Dr. Barr. “With both progesterone and testosterone also low, there is less sebaceous gland activity and oil production, contributing to skin dryness.”
Cumulatively, this can all add up to dehydrated skin that’s more prone to irritation and inflammation. According to Dr. Barr, this is why conditions like atopic dermatitis (eczema), contact dermatitis, and psoriasis, may be worse just before or during your period.
What you can do: Moisturizing with soothing and nourishing skincare ingredients is often your best bet. Opt for gentle cleansers and look for things like hyaluronic acid, ceramides, gotu kola, and sea buckthorn oil on ingredient lists, suggests Dr. Barr. Scaling back on abrasive exfoliants and products containing too many active ingredients, including topical retinoids and chemical exfoliants, may also help if you’re prone to irritation. Finally, drinking plenty of water and eating foods rich in omega-3 fats, vitamin C, and antioxidants can help ease inflammation and irritation, support a healthy skin barrier, and promote hydration from the inside out.
Follicular phase (days 1-14)
After your period, the remainder of your follicular phase is characterized by increases in estrogen levels, which peak around day 14 (when most women ovulate). “This translates to a boost in skin barrier function, skin hydration, hyaluronic acid production, and collagen production,” says Dr. Barr. “Skin is typically smoother, calmer, and more radiant than other times of the month, as estrogen peaks at ovulation and progesterone is still low, which means those sebaceous glands are pumping out less oil.”
What you can do: You don’t need to do much at all! This is a time to embrace your natural glow and take a break from makeup—but don’t forget your moisturizer with SPF—due to estrogen’s effect on pigment-producing cells, you want to be sure to protect your skin from UV rays, warns Dr. Barr. Using products with more active ingredients such as alpha-hydroxy acids (e.g. glycolic acid, lactic acid) and retinoids is usually better tolerated during this time of the month since skin barrier function is optimal.
Luteal Phase (days 15-28)
Here’s when things can get a little…greasy. When you ovulate on day 14, there is a surge in luteinizing hormone (LH), which prompts a rise in progesterone and testosterone, and “these two hormones contribute to increased sebaceous gland activity and oilier skin, including an oily scalp,” says Dr. Barr. “Additionally, estrogen levels are low relative to progesterone, so there may be more inflammation, irritation, and disruption of the skin barrier, which may contribute to breakouts.”
In fact, 60-70 percent of women experience these mild premenstrual flares of acne. The lower half of the cheeks, the chin, and the jawline region are the most common areas for these hormonal acne breakouts, says Zenovia Gabriel, MD, FAAD, who specializes in hormonal dermatology.
Towards the end of the luteal phase, estrogen continues to decline and progesterone decreases as well, transitioning your skin to that dryer, more dehydrated, inflamed state that can be typical during menstruation, as previously discussed.
What you can do: If you notice that your skin is more oily and prone to acne, adding a toner after cleansing may be helpful. Look for ingredients like salicylic acid, benzoyl peroxide, tea tree oil, and witch hazel, which may help kill the bacteria associated with acne and accelerate cellular turnover. But don’t go overboard with products that strip the skin of oil, cautions Dr. Barr, as this could actually cause your skin to oversecrete oil.
Acne is also a very inflammatory condition, so nourishing your body with anti-inflammatory foods rich in omega-3 fats, vitamin C, and antioxidants may be beneficial, as well as scaling back on added sugars and dairy, since these have both been linked to hormonal breakouts. Getting good sleep, exercising, meditating, and connecting with friends and family are all activities that can help curb inflammation as well, says Dr. Barr.
Other factors in your 20s and 30s

In addition to these “typical” hormonal shifts that most women in their 20s and 30s experience, other factors can affect hormones and thus skin health—namely, birth control pills and stress.
Hormonal birth control comes in many forms, but often, doctors prescribe combined oral hormonal contraceptives—pills that contain synthetic forms of both estrogen and progesterone, especially for women struggling with acne, menstrual cramps, or irregular periods. The data shows that combined contraceptives, as a class, exhibit a pro-estrogen effect on the skin and reduce the production of androgens, making them helpful for these issues, says Dr. Zenovia. However, it’s important to note that once someone stops taking birth control, these issues will often reemerge as they don’t get to the root of any potential hormonal imbalances.
Your 20s and 30s are often packed with particularly stressful transition periods as well (think: entering the workforce, navigating new relationships, having babies, etc). Research has shown that psychological stress can negatively impact skin barrier function, which, in turn, may trigger or exacerbate eczema, psoriasis, acne, and overall skin irritation. This may be due to elevated levels of the stress hormone cortisol, which is associated with inflammation and inflammatory skin conditions. So, anything you can do to curb the effects of stress—exercising, meditating, talking to a therapist—may help your skin, too.
Pregnancy

During pregnancy, increased levels of estrogen and progesterone lead to increases in melanin stimulating hormone (MSH), which stimulates pigment cells called melanocytes. This, in turn, can contribute to darker moles, darker nipples, a darker vulva, and even melasma says Dr. Zenovia. Melasma during pregnancy is called chloasma. It affects about 45–75 percent of pregnant women and is characterized by patchy brown spots often occurring on the forehead, upper lip, and cheeks due to increased production of melanin by melanocytes.
For some women, pregnancy may also increase sebum production, which may or may not lead to acne. During pregnancy, the body also increases blood production by about 50 percent, which may boost circulation and contribute to an overall brighter complexion. Together, these factors may contribute to that dewy, rosy so-called pregnancy glow.
What you can do: Pregnancy-induced melasma is directly stimulated and worsened by UV exposure, so it’s crucial to reduce your sun exposure, wear protective clothing, or use a physical (a.k.a. mineral-based) sunscreen, says Dr. Zenovia. If your melasma is minor, it will typically resolve postpartum. If you happen to experience acne, your options are a bit limited during pregnancy, but The American College of Obstetricians and Gynecologists says it’s safe to use topical glycolic acid, azelaic acid, benzoyl peroxide, and salicylic acid.
In your 40s and 50s
Depending on your health and your hormones, your 40s might look a lot like your 30s. If you’re menstruating regularly, many of the cyclical hormonal fluctuations and recommendations above will still apply to you. Likewise, if you’re pregnant in your 40s, check out the tips above.
However, for many women, their 40s are characterized by irregular periods and fluctuations in estrogen and progesterone levels that eventually lead to significant drops in these hormones. This transition period is called perimenopause, and once you’ve gone through 12 consecutive months without a period, you’ve officially reached menopause. Most women hit menopause between age 45 and 50, with an average age of 51.
“When our hormones [estrogen and progesterone] diminish during perimenopause and postmenopause, the functions they perform to maintain the health and vitality of the skin diminish as well,” says Dr. Barr.
The skin is full of estrogen receptors, and when estrogen binds to those receptors, it stimulates the production of hyaluronic acid, which enhances hydration and plumps skin, as well as the synthesis of collagen and elastin, which contribute to skin’s firmness and resiliency. “But without estrogen’s influence, pores will appear larger and fine lines, wrinkles, and sagging skin becomes more prominent,” says Dr. Barr. In fact, research suggests that women lose around 30 percent of their collagen in the five years following menopause, so the changes can be quite significant.
But that’s not all. There’s also a decline in sebum production and circulation that can alter the skin’s barrier, resulting in skin that’s dry, sensitive, and prone to irritation and inflammation, according to Dr. Barr. Skin cellular turnover (how quickly skin cells can replace themselves) also declines, which not only gives skin a generally dull appearance but contributes to slower wound healing and age spots. Skin also has a reduced ability to handle oxidative damage from sun exposure, which can increase skin cancer risk.
What you can do: While there’s a lot that’s seemingly going wrong with your skin during this time, there’s also a lot you can do! First and foremost, due to your skin’s reduced ability to handle oxidative stress, using sunscreen daily is a must.
To battle dryness, you’ll also want to use gentle, non-foaming cleansers and products with soothing and nourishing skincare ingredients, including hyaluronic acid, ceramides, gotu kola, and sea buckthorn oil, suggests Dr. Barr. Drinking plenty of water and eating foods rich in omega-3 fats, vitamin C, and antioxidants can also help ease inflammation and promote hydration. Some research even suggests that oral collagen supplements can improve skin’s moisture levels and elasticity.
To support skin cell turnover and enhance collagen production, consider trying a topical retinol product, suggests Dr. Zenovia. Retinol increases the turnover rate of keratinocytes, which helps skin appear smoother and dewier, and helps unclog pores. Over time, research shows it can support collagen production in the dermis and inhibit the breakdown of collagen. However, retinol can be irritating for some people and it increases your skin’s sensitivity to the sun. For something gentler, consider a serum or cream containing the plant-derived ingredient bakuchiol, which supports skin cell turnover without increasing photosensitivity.
The Takeaway

Your skin and hormones are connected, so as your hormone levels change throughout your life, knowing how those changes affect your skin can help you look and feel your best. Don’t be intimidated by these different stages—there are plenty of products and lifestyle changes that can help your skin thrive.

This Menopause Supplement Will Help You Cool Down and Feel More You Again

Is Your Skin Dehydrated or Dry? Here’s How to Tell and Treat It

5 Naturally High-Collagen Foods & 19 Foods That Boost Collagen Levels for Super Supple Skin & Joints





