MENOPAUSE SYMPTOMS. Let’s talk about it...
Between 2014 and 2025, 1.1 billion women will have gone through menopause. To put that into perspective, the U.S. currently has around 169 million females. Suffice it to say, (postmenopausal) women run the world. Yet, 60 percent of women say the physical and mental effects of declining hormone levels aren’t discussed enough, leaving them feeling unprepared for menopause.
That’s why it’s no surprise nearly 90 percent of women go to their doctor for advice on coping with menopause-related symptoms. The kicker? 7 in 10 women have not received any treatment for their symptoms. But you don’t have to suffer in silence.
Get to know what’s really happening during menopause, what causes menopause symptoms, and how to get relief from menopause symptoms.
What is Menopause?
While the word menopause is often used to describe the symptomatic time leading up to the end of menstrual cycles, technically menopause is just one day. Menopause is defined as the day that it’s been 12 consecutive months since a person’s last period. Every person with a uterus will go through menopause.
“The main shift in menopause centers on a decrease in ovarian follicles, creating a drop in estrogen and progesterone,” explains Shoma Datta-Thomas, MD, FACOG, a board-certified gynecologist with Maiden Lane Medical and NY Presbyterian Hospital – Weill Cornell. “This sets into motion changes in other hormones which help maintain the menstrual cycle.”
When Does Menopause Start?
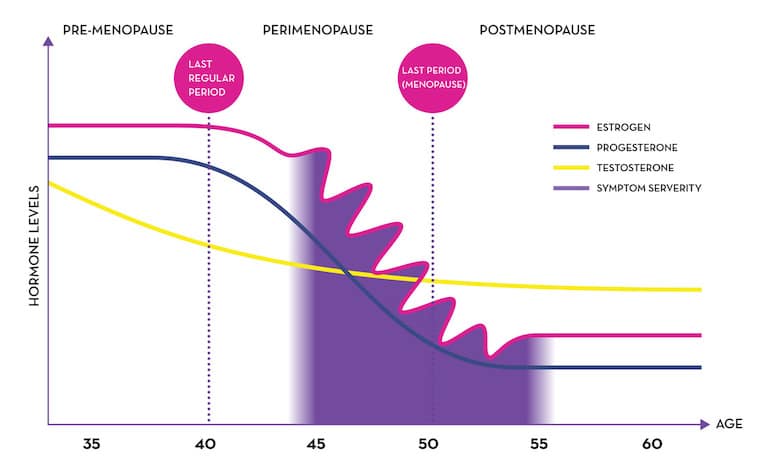
The average age of menopause in the U.S. is 51, but it can happen from around 40-58. The gradual shift in hormones leading up to menopause is called perimenopause. Perimenopause typically starts in 40s and lasts an average of 4-8 years.
Learn more about what happens at each stage of menopause below.
Stages of Menopause
Perimenopause
- Estrogen begins to decline and fluctuates
- Periods can occur less often
- Cycle flow and duration shifts
- Still possible to get pregnant
- Early-stage: Period differs by 7 or more days each cycle
- Late-stage: Cycles become >60 days apart
- Ovarian reserve is low
- Menopausal symptoms begin
Menopause
- After periods have stopped for 12 straight months
- Ovaries stop producing estrogen and releasing eggs
- Can no longer become pregnant
- Menopausal symptoms continue
Postmenopause
- 1 year since last period
- Increased bone loss
- Increased risk of bone and heart conditions
- Some symptoms may continue

Common Menopause Symptoms
While every woman will experience menopause differently, these are a few of the most common symptoms.
- Hot flashes
- Night sweats
- Vaginal dryness
- Bladder problems
- Joint and muscle discomfort
- Low sex drive
- Sleep issues
- Fatigue
- Mood swings
- Irritability
- Restlessness
- Heart racing
How Long Do Menopause Symptoms Last?
Menopause symptoms usually fluctuate in the 4-8 years leading up to menopause, but in some women, they could last beyond that, post-menopause. “Initially, it was thought hot flashes stopped within a few years after the last period but now there is evidence it can last even a decade or more,” says Dr. Datta-Thomas. These variations may also vary by race, she points out. Research has found that Black women are more likely to experience hot flashes for more than five years.
Causes of Menopause Symptoms and How to Get Natural Menopause Relief
Hot flashes and night sweats
Why it happens: Estrogen receptors can be found in the area of the brain that controls a process called thermoregulation, or temperature regulation. Estrogen also directly controls the diameter of blood vessels and can make them dilate, or get bigger (known as vasodilation), which leads to more blood flow and sweating. “Hot flashes can be experienced very differently by individual women,” says Dr. Datta-Thomas. But it usually starts with “a hot flushed feeling that often starts at the chest and face, then spreads.” It can include sweating, the feeling of a racing heart, shivering, and even and a feeling of doom, she explains.
What you can do: Stock up on soy.
Soy products like tofu, edamame, soy nuts, and soy milk contain soy isoflavones, a chemical compound that mimics estrogen. Consuming soy isoflavones can help reduce the short-term frequency and severity of hot flashes in some women.
Limit triggering foods.
“This is an important time to limit triggers like spicy foods and focus on a heart-healthy diet with low fat, salt, and sugar,” says Dr. Datta-Thomas. Caffeine and alcohol can also be triggers for some women. Keeping a log of what you’ve had to eat or drink may help you pinpoint triggers.
Vaginal dryness
Why it happens: Pre-menopause, estrogen helps to circulate blood to the vagina, keeping the tissue healthy and elastic, explains Mache Seibel, MD, OB-GYN, Harvard Medical School faculty and author of The Estrogen Fix. The blood flow also aids in vaginal lubrication. “Vaginal moisture is like the equivalent of sweat,” says Dr. Seibel. “It goes through the wall of the vagina just like sweat goes through your skin. With reduced blood flow there is less fluid created that can transfer through the wall into the vagina.” The result? The most outer layer of the vagina, called the mucosa, begins to thin and dry, making sex painful.
What you can do:
Have more sex.
Whether with a partner or on your own, stimulating the vagina can actually help to maintain healthy vaginal tissue by increasing blood flow to the area, says Dr. Seibel. While it may sound counterintuitive (see: low sex drive), think of the vagina like you would any other muscle: you gotta work.
Learn to love lube.
Maybe you’ve never used a lubricant before, but there’s no shame in starting now. There are two main over-the-counter options to try, says Dr. Seibel: Moisturizers are able to maintain moisture over time, whereas lubricants can help in the moment. While silicone-based products last longer than water-based ones, just be aware that when they wash off in the shower, things can get extra slippery.
Bladder problems
Why it happens: Research shows estrogen improves muscle mass and increases the collagen content of connective tissues. Dipping estrogen levels can weaken the pelvic floor muscles, affecting the bladder and urethra and leading to leakage. It can also lead to a more sensitive bladder. Think: getting up in the middle of the night to pee, having to go more frequently, and having little warning before you need to go. Petition to give menopausal women the aisle seat, always? We co-sign.
What you can do:
Try pelvic floor therapy
Strengthening the pelvic floor muscles can improve bladder function, no matter what stage of menopause you’re in. “Changes associated with our posture, exercise, pregnancy and natural aging can affect the pelvic floor and physical therapy can really help,” says Dr. Datta-Thomas. Bonus: It may also help to address discomfort during sex, she says.
Avoid natural diuretics.
“In general, caffeinated beverages and alcohol act as diuretics and promote urine production,” explains Dr. Datta-Thomas. This can make it even more difficult when you’re dealing with that always-gotta-go feeling. “As with healthy diet changes I don’t want you to cut out all the ‘good stuff,’ but really try to identify what helps or hurts your symptoms,” she says. Knowing how certain food or drinks impact you can help you plan ahead while still enjoying them.
Low sex drive
Why it happens: Your trifecta of sex hormones—estrogen, progesterone, and testosterone—all play a role in libido, so declines in all three hormones throughout the phases of menopause can leave you less than revved up. Plus, if you’re not sleeping well, dealing with hot flashes, and know it may be painful, there’s little chance you’ll feel in the mood, says Dr. Seibel.
What you can do:
Slow things down.
Women’s sex response relies more on emotional intimacy than men’s, explains Dr. Seibel. That means it can take more time to get warmed up. Be open with your partner about investing time to meet your needs. Build in time for foreplay, don’t pressure yourself to squeeze in a quickie, and remember that you don’t have to orgasm to enjoy yourself.
Try a toy.
Whether you add a sex toy, such as a vibrator, into your foreplay or use it to get the job done, the novelty alone can help to rev up your sex drive. Vibrators can also help to stimulate lubrication, getting you more in the mood, and provide different sensations that might hit the spot.
Sleep issues and fatigue
Why it happens: “Estrogen helps to maintain the rapid eye movement, or REM, sleep,” says Dr. Seibel. This stage of sleep is restorative and important for learning and memory. “REM is shortened in the absence or reduction of estrogen,” he explains, leading many women to wake up from a full night of sleep yet still feel tired. Scientists also discovered that decreases in estradiol, a type of estrogen, were associated with higher odds of trouble falling asleep and waking up at night. Increases in follicle-stimulating hormone (FSH), which occurs during late-stage perimenopause, were also associated with nighttime waking. It’s no wonder if you’re feeling drained.
On top of that, sleep problems can be related to the stress of going through perimenopause and the symptoms that go with it: Women who experience hot flashes and night sweats are more likely to report sleep difficulty, finds research in the journal Sleep.
What you can do:
Commit to a schedule.
The more consistent your sleep pattern, the better, says Dr. Seibel. Going to bed at the same time every night and waking up at the same time can help to train your circadian rhythm, so your body will be more primed for sleep. Choose times that can work for you both on weekdays and the weekend to avoid throwing off your rhythm.
Amp up the aerobics.
Walking, biking, or using a treadmill for 30-40 minutes four times a week improve sleep quality, daytime sleepiness, and vitality in women over 55, shows research. To get the most benefit, make sure two sessions a week are at an effort where you can only speak about one to two sentences and your breathing is heavier. Regular, weight-bearing exercise may also help with the joint and muscle pain that some women experience, says Dr. Datta-Thomas.
Stretch, then snooze.
After you brush your teeth, add this to your routine: stretching for just 10 minutes before bed helped women fall asleep faster, found research. In a similar study, women who got flexy before bed reported an overall decrease in menopause-related symptoms, including sleep disturbances.
Mood swings, irritability, and restlessness
Why it happens: “The lowering of estrogen in the brain, and progesterone to some extent, is going to change the dynamics of brain chemistry in a way that is less calming and less mood-enhancing,” says Dr. Seibel. Specifically, the inhibitory neurotransmitters serotonin and GABA, which are known for stabilizing mood, decline.
What you can do:
Remember this is totally normal.
The simple step of acknowledging that what you’re experiencing may be tied to menopause can bring a sense of relief, explains Dr. Seibel. “A lot of women who are going through this get worried they are having dementia or that they are no longer the person they used to be.” You’re still you, you’re not alone, and there are solutions to help you through this.
Hone in on your diet.
What you eat can play a big part in your mood—90 percent of your body’s serotonin is actually made in the gut! Aim for a variety of foods high in nutrients, like fruits and vegetables, lean protein, and whole grains. Probiotic foods, like kimchi, sauerkraut, and yogurt can also help to modulate mood via the gut-brain axis. And while research is still ongoing, eating foods rich in the amino acid tryptophan, like turkey, eggs, and salmon, may help boost serotonin levels. (These 7 foods are great for perimenopause)
Start a mindfulness practice.
If you’re not already meditation, this may convince you: Women with higher mindfulness scores had fewer menopausal symptoms overall, including mood changes and irritability. Mindfulness can include stopping to take a few deep breaths, doing a guided meditation, or even journaling.
The Takeaway
Remember there are so many other women going through exactly the same thing and you are not alone. If you’re looking for extra support during your menopause journey, HUM’s Fan Club is an estrogen-free, non-hormonal, menopause supplement designed to help with 11 symptoms of perimenopause and menopause.









